EXPLAINED: Everything you need to know about Switzerland’s Covid-19 vaccination rollout
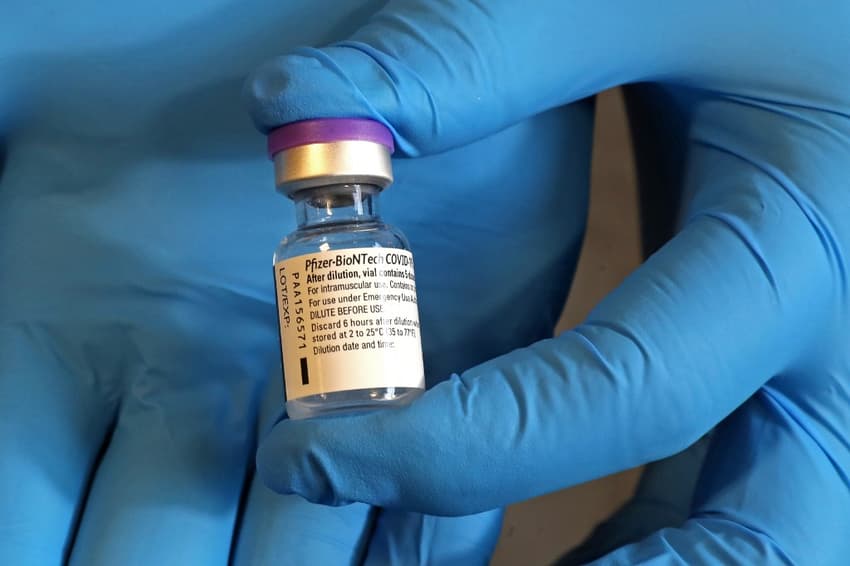
Switzerland has begun rolling out the coronavirus vaccine. Here's what you need to know.
The Swissmedic regulatory authority approved the Pfizer-BioNTech Covid-19 vaccine for use in Switzerland on December 21st. Vaccinations started in Switzerland on December 23rd.
How was the vaccine approved?
The Federal Office of Public Health (FOPH) had been planning to start vaccinating by the end of January.
However, Swissmedic finished its rolling review of the vaccine sooner than thought, allowing Switzerland to begin vaccinating before the end of the year.
“After a meticulous review of the available information, Swissmedic concluded that the COVID-19 vaccine from Pfizer/BioNTech is safe and that its benefit outweighs the risks”, the agency said in a statement on Friday.
It added that the approval of the vaccine in Switzerland “is the first in the world to be granted in a regular process” rather than through the emergency authorisation, as was the case in the United States and the UK.
"We were surprised by the speed of the authorisation and the imminent arrival of vaccine doses," Secretary General of the Conference of Cantonal Directors of Health Michael Jordi told reporters on Saturday.
The military, which is in charge of the vaccine storage and transport, will deliver nearly 107,000 doses in the coming days, then 250,000 per month as of January, according to Daniel Aeschbach, the army's chief pharmacist.
READ MORE: Vaccinations to start in Switzerland 'within days' after official approval
Which cantons will vaccinate first?
As it stands now, the vaccination programme — which will be free and voluntary — will begin this week in Uri, Schwyz, Nidwalden, Obwalden, Lucerne, Zug, Fribourg, and Valais, 20 Minuten news site reported.
Basel City is planning to commence on the week of December 28th, followed by the other Swiss cantons from January 4th.
READ: When will coronavirus vaccinations start in your Swiss canton?
The cantons are still scrambling to set up special vaccination units, which may include gyms, civil protection facilities, and exhibition centres — large venues allowing to vaccinate as many people as possible at one time.
Hospitals, doctors’ practices and pharmacies will be able to vaccinate people as well, though on a less massive scale.
What will be the rollout process throughout Switzerland?
Launching a vaccination programme “is extremely complicated logistically”, Swiss Health Minister Alain Berset said.
This is due to the infrastructure that must be set up to store, distribute and administer the vaccines.
“In recent months, we have prepared infrastructures with ultra-cold warehouses,” Aeschbach said.
"Once the vaccines are delivered, storage and vaccination will be the responsibility of cantonal authorities".
If necessary, the military will also provide ice to safely store the doses, as most locations don’t have specialised freezers needed to keep the highly perishable vaccines at extremely low temperatures.
The Pfizer vaccine, for instance, has to be kept at -80 degrees Celsius.
How many vaccines have the Swiss ordered and how will they be administered?
The government’s Covid-19 vaccination strategy involves the distribution of the approximately 13 million doses from three manufacturers: Moderna (4.5 million doses), AstraZeneca (5.3 million) and Pfizer (3 million ).
That is enough to vaccinate 6 million people out of Switzerland’s total population of about 8.6 million, as the vaccine has to be given in two doses, about three weeks apart.
“Each vial contains ten doses. The strategy is to minimise loss associated with repartitioning each vial”, Giuseppe Pantaleo, head of the Department of Laboratory Medicine and Pathology at Vaud’s University Hospital (CHUV), told RTS public broadcaster.
This means having ten people available within three hours to use all the doses.
“The challenge is not mass vaccination, but to immunise such a large number of people in an extremely limited time”, Pantaleo said.
READ MORE: Switzerland reveals its Covid-19 vaccination strategy
Who will be vaccinated first?
Once the inoculation program starts this month, groups at risk would be vaccinated first. They include essential healthcare workers, the elderly, as well as people with diabetes, chronic lung disease and high blood pressure.
The second group to be vaccinated are health care workers who are in daily contact with patients, and those who take care of ‘vulnerable’ people — for instance, employees of elderly care homes.
Next will be people living in the same household as at-risk individuals.
The fourth group will consist of those residing or working in community institutions that present a heightened risk of infection or potential for an outbreak, like institutions for people with disabilities.
The last group will be members of general public who want to be vaccinated.
FOPH estimates that the whole process will probably last until the summer.
Comments
See Also
The Swissmedic regulatory authority approved the Pfizer-BioNTech Covid-19 vaccine for use in Switzerland on December 21st. Vaccinations started in Switzerland on December 23rd.
How was the vaccine approved?
The Federal Office of Public Health (FOPH) had been planning to start vaccinating by the end of January.
However, Swissmedic finished its rolling review of the vaccine sooner than thought, allowing Switzerland to begin vaccinating before the end of the year.
“After a meticulous review of the available information, Swissmedic concluded that the COVID-19 vaccine from Pfizer/BioNTech is safe and that its benefit outweighs the risks”, the agency said in a statement on Friday.
It added that the approval of the vaccine in Switzerland “is the first in the world to be granted in a regular process” rather than through the emergency authorisation, as was the case in the United States and the UK.
"We were surprised by the speed of the authorisation and the imminent arrival of vaccine doses," Secretary General of the Conference of Cantonal Directors of Health Michael Jordi told reporters on Saturday.
The military, which is in charge of the vaccine storage and transport, will deliver nearly 107,000 doses in the coming days, then 250,000 per month as of January, according to Daniel Aeschbach, the army's chief pharmacist.
READ MORE: Vaccinations to start in Switzerland 'within days' after official approval
Which cantons will vaccinate first?
As it stands now, the vaccination programme — which will be free and voluntary — will begin this week in Uri, Schwyz, Nidwalden, Obwalden, Lucerne, Zug, Fribourg, and Valais, 20 Minuten news site reported.
Basel City is planning to commence on the week of December 28th, followed by the other Swiss cantons from January 4th.
READ: When will coronavirus vaccinations start in your Swiss canton?
The cantons are still scrambling to set up special vaccination units, which may include gyms, civil protection facilities, and exhibition centres — large venues allowing to vaccinate as many people as possible at one time.
Hospitals, doctors’ practices and pharmacies will be able to vaccinate people as well, though on a less massive scale.
What will be the rollout process throughout Switzerland?
Launching a vaccination programme “is extremely complicated logistically”, Swiss Health Minister Alain Berset said.
This is due to the infrastructure that must be set up to store, distribute and administer the vaccines.
“In recent months, we have prepared infrastructures with ultra-cold warehouses,” Aeschbach said.
"Once the vaccines are delivered, storage and vaccination will be the responsibility of cantonal authorities".
If necessary, the military will also provide ice to safely store the doses, as most locations don’t have specialised freezers needed to keep the highly perishable vaccines at extremely low temperatures.
The Pfizer vaccine, for instance, has to be kept at -80 degrees Celsius.
How many vaccines have the Swiss ordered and how will they be administered?
The government’s Covid-19 vaccination strategy involves the distribution of the approximately 13 million doses from three manufacturers: Moderna (4.5 million doses), AstraZeneca (5.3 million) and Pfizer (3 million ).
That is enough to vaccinate 6 million people out of Switzerland’s total population of about 8.6 million, as the vaccine has to be given in two doses, about three weeks apart.
“Each vial contains ten doses. The strategy is to minimise loss associated with repartitioning each vial”, Giuseppe Pantaleo, head of the Department of Laboratory Medicine and Pathology at Vaud’s University Hospital (CHUV), told RTS public broadcaster.
This means having ten people available within three hours to use all the doses.
“The challenge is not mass vaccination, but to immunise such a large number of people in an extremely limited time”, Pantaleo said.
READ MORE: Switzerland reveals its Covid-19 vaccination strategy
Who will be vaccinated first?
Once the inoculation program starts this month, groups at risk would be vaccinated first. They include essential healthcare workers, the elderly, as well as people with diabetes, chronic lung disease and high blood pressure.
The second group to be vaccinated are health care workers who are in daily contact with patients, and those who take care of ‘vulnerable’ people — for instance, employees of elderly care homes.
Next will be people living in the same household as at-risk individuals.
The fourth group will consist of those residing or working in community institutions that present a heightened risk of infection or potential for an outbreak, like institutions for people with disabilities.
The last group will be members of general public who want to be vaccinated.
FOPH estimates that the whole process will probably last until the summer.
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.